Fighting Fallen Arches

?Life begins at 40,? goes an old quote, ?and so do fallen arches.? It?s time to toss that negative idea out the window and get the real facts on fallen arches and what you can do about them. We have all seen what our footprints look like as we walked across sand or left a water trail after getting out of the bathtub. The narrow part of the footprint is where your natural arch exists. What gives you that arch are tendons that pull together to create an upward curve. When your tendons are not properly pulling together, you start to lose that natural arch. This condition is known as flat foot or fallen arch.
Causes
Abnormal development of the foot, producing Pes Planus, may be due to neurological problems, eg cerebral palsy, polio. Bony or ligamentous abnormalities, eg tarsal coalition (fusion of tarsal bones), accessory navicular bone. A small proportion of flexible flat feet do not correct with growth. Some of these may become rigid if the Pes Planus leads to bony changes.
Symptoms
Many people have flat feet and notice no problems and require no treatment. But others may experience the following symptoms, Feet tire easily, painful or achy feet, especially in the areas of the arches and heels, the inside bottom of your feet become swollen, foot movement, such as standing on your toes, is difficult, back and leg pain, If you notice any of these symptoms, it's time for a trip to the doctor.
Diagnosis
If you notice that your feet are flat, but you?re not really experiencing any pain, then you?re probably okay to go without a visit to the podiatrist (unless, of course, you have a lack of feeling in your foot). You can schedule a hair appointment instead, or maybe see a movie. However, once painful symptoms start to appear, it?s better to skip the hirsute (or cinematic) experience and go see your foot doctor. Your podiatrist will likely make the diagnosis by examining your foot visually, asking about symptoms you may be experiencing, and may test your muscle strength. You may be asked to stand on your toes (in a ballerina pose, if you prefer, although that?s certainly not required), or walk around the examining room, and you may need to show the podiatrist your shoes. He or she may comment on your excellent taste in footwear, but is more likely to check your shoes for signs of wear that may indicate fallen arches. Your podiatrist may recommend X-rays, a CT scan or an MRI in order to get a look at the interior of your foot, although the best diagnosis usually comes from the doctor?s own in-person examination.
heelsncleavage
Non Surgical Treatment
The type of treatment will depend on the stage of PTTD present. There are four stages of posterior tibial tendon dysfunction. Stage I. The posterior tibial tendon is inflamed but has normal strength. There is little to no change in the arch of the foot. The patient can still perform a single-limb heel rise and has a flexible hindfoot. Orthotic treatment options include modified off the shelf inserts and custom molded orthotics. Stage 2. The tendon is partially torn or shows degenerative changes and as a result loses strength.There is considerable flattening of the arch without arthritic changes in the foot. The patient cannot perform single-limb heel rise. Pain is now present on the lateral aspect of the ankle. Orthotic treatment is similar as that in stage I, with the addition of more rigid arch supports and wedging. Stage 3. Results when the posterior tibial tendon is torn and not functioning. As a result the arch is completely collapsed with arthritic changes in the foot. A solid ankle AFO is suggested in conjunction with a modified orthopedic shoe. Stage 4. Is identical to stage three except that the ankle joint also becomes arthritic. A rigid AFO and modified orthopedic shoe is required.
Surgical Treatment

Feet that do not respond to the treatments above may need surgery. The surgery will help to create a supportive arch.
Everything It Is Best To Understand About

Plantar fasciitis is an inflammation of the long band of connective tissue running from the heel to the ball of the foot. The plantar fascia acts like a bowstring and supports the arch and several muscles inside the foot. When there is increased stress on the arch, microscopic tears can occur within the plantar fascia, usually at its attachment on the heel. This results in inflammation and pain with standing and walking and sometimes at rest.
Causes
To understand the cause of the pain one must understand the anatomy of the foot and some basic mechanics in the function of the foot. A thick ligament, called the plantar fascia, is attached into the bottom of the heel and fans out into the ball of the foot, attaching into the base of the toes. The plantar fascia is made of dense, fibrous connective tissue that will stretch very little. It acts something like a shock absorber. As the foot impacts the ground with each step, it flattens out lengthening the foot. This action pulls on the plantar fascia, which stretches slightly. When the heel comes off the ground the tension on the ligament is released. Anything that causes the foot to flatten excessively will cause the plantar fascia to stretch greater that it is accustom to doing. One consequence of this is the development of small tears where the ligament attaches into the heel bone. When these small tears occur, a very small amount of bleeding occurs and the tension of the plantar fascia on the heel bone produces a spur on the bottom of the heel to form. Pain experienced in the bottom of the heel is not produced by the presence of the spur. The pain is due to excessive tension of the plantar fascia as it tears from its attachment into the heel bone. Heel spur formation is secondary to the excessive pull of the plantar fascia where it attaches to the heel bone. Many people have heel spurs at the attachment of the plantar fascia with out having any symptoms or pain. There are some less common causes of heel pain but they are relatively uncommon. There are several factors that cause the foot to flatten and excessively stretching the plantar fascia. The primary factor is the structure of a joint complex below the ankle joint, called the subtalar joint. The movement of this joint complex causes the arch of the foot to flatten and to heighten. Flattening of the arch of the foot is termed pronation and heightening of the arch is called supination. If there is excessive pronation of the foot during walking and standing, the plantar fascia is strained. Over time, this will cause a weakening of the ligament where it attaches into the heel bone, causing pain. When a person is at rest and off of their feet, the plantar fascia attempts to mend itself. Then, with the first few steps the fascia re-tears causing pain. Generally, after the first few steps the pain diminishes. This is why the heel pain tends to be worse the first few steps in the morning or after rest. Another factor that contributes to the flattening of the arch of the foot is tightness of the calf muscles. The calf muscle attaches into the foot by the achilles tendon into the back of the heel. When the calf muscle is tight it limits the movement of the ankle joint. When ankle joint motion is limited by the tightness of the calf muscle it forces the subtalar joint to pronate excessively. Excessive subtalar joint pronation can cause several different problems to occur in the foot. In this instance, it results in excessive tension of the plantar fascia. Tightness of the calf muscles can be a result of several different factors. Exercise, such as walking or jogging will cause the calf muscle to tighten. Inactivity or prolonged rest will also cause the calf muscle to tighten. Women who wear high heels and men who wear western style cowboy boots will, over time, develop tightness in the calf muscles.
Symptoms
Symptoms may also include swelling that is quite tender to the touch. Standing, walking and constrictive shoe wear typically aggravate symptoms. Many patients with this problem are middle-aged and may be slightly overweight. Another group of patients who suffer from this condition are young, active runners.
Diagnosis
A biomechanical exam by your podiatrist will help reveal these abnormalities and in turn resolve the cause of plantar fasciitis. By addressing this cause, the patient can be offered a podiatric long-term solution to his problem.
Non Surgical Treatment
Treatment of heel pain depends on its cause. Plantar fasciitis. Most doctors recommend a six- to eight-week program of conservative treatment, including temporary rest from sports that trigger the foot problem, stretching exercises, ice massage to the sole of the foot, footwear modifications, taping of the sole of the injured foot, and acetaminophen (Tylenol) or nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin or ibuprofen (Advil, Motrin and others) for pain. If this conservative treatment doesn't help, your doctor may recommend that you wear a night splint or a short leg cast, or he or she may inject corticosteroid medication into the painful area. Surgery is rarely necessary and is not always successful. Heel spur. Conservative treatment includes the use of shoe supports (either a heel raise or a donut-shaped heel cushion) and a limited number of local corticosteroid injections (usually up to three per year). As in plantar fasciitis, surgery is a last resort. Calcaneal apophysitis. This condition usually goes away on its own. In the meantime, conservative treatment includes rest and the use of heel pads and heel cushions. Bursitis. Treatment is similar to the treatment of heel spurs. Changing the type of footwear may be essential.
Surgical Treatment
Surgery is a last resort in the treatment of heel pain. Physicians have developed many procedures in the last 100 years to try to cure heel pain. Most procedures that are commonly used today focus on several areas, remove the bone spur (if one is present), release the plantar fascia (plantar fasciotomy), release pressure on the small nerves in the area. Usually the procedure is done through a small incision on the inside edge of the foot, although some surgeons now perform this type of surgery using an endoscope. An endoscope is a tiny TV camera that can be inserted into a joint or under the skin to allow the surgeon to see the structures involved in the surgery. By using the endoscope, a surgeon can complete the surgery with a smaller incision and presumably less damage to normal tissues. It is unclear whether an endoscopic procedure for this condition is better than the traditional small incision. Surgery usually involves identifying the area where the plantar fascia attaches to the heel and releasing the fascia partially from the bone. If a small spur is present this is removed. The small nerves that travel under the plantar fascia are identified and released from anything that seems to be causing pressure on the nerves. This surgery can usually be done on an outpatient basis. This means you can leave the hospital the same day.
pain in back of heel
Prevention

A variety of steps can be taken to avoid heel pain and accompanying afflictions. Wear shoes that fit well-front, back, and sides-and have shock-absorbent soles, rigid shanks, and supportive heel counters. Wear the proper shoes for each activity. Do not wear shoes with excessive wear on heels or soles. Prepare properly before exercising. Warm up and do stretching exercises before and after running. Pace yourself when you participate in athletic activities. Don?t underestimate your body's need for rest and good nutrition. If obese, lose weight.
Acceptable Leg Length Discrepancy After Hip Replacement
People with leg length discrepancy, when one leg is longer than the other, usually have a waddling-type gait where the hips seem to move up and down during walking as the body tries to compensate for the inequality. There are two types of leg length discrepancy. The first type of leg length discrepancy involves a structural defect, where one bone is longer or shorter than the corresponding bone of the other limb. This can occur within the femur (upper leg bone) or the tibia and fibular (lower leg bones). Functional leg length discrepancy results from altered mechanics due to a malalignment in the spine or lower extremity.

Causes
Some children are born with absence or underdeveloped bones in the lower limbs e.g., congenital hemimelia. Others have a condition called hemihypertrophy that causes one side of the body to grow faster than the other. Sometimes, increased blood flow to one limb (as in a hemangioma or blood vessel tumor) stimulates growth to the limb. In other cases, injury or infection involving the epiphyseal plate (growth plate) of the femur or tibia inhibits or stops altogether the growth of the bone. Fractures healing in an overlapped position, even if the epiphyseal plate is not involved, can also cause limb length discrepancy. Neuromuscular problems like polio can also cause profound discrepancies, but thankfully, uncommon. Lastly, Wilms? tumor of the kidney in a child can cause hypertrophy of the lower limb on the same side. It is therefore important in a young child with hemihypertrophy to have an abdominal ultrasound exam done to rule out Wilms? tumor. It is important to distinguish true leg length discrepancy from apparent leg length discrepancy. Apparent discrepancy is due to an instability of the hip, that allows the proximal femur to migrate proximally, or due to an adduction or abduction contracture of the hip that causes pelvic obliquity, so that one hip is higher than the other. When the patient stands, it gives the impression of leg length discrepancy, when the problem is actually in the hip.
Symptoms
The effects of limb length discrepancy vary from patient to patient, depending on the cause and size of the difference. Differences of 3 1/2 percent to 4 percent of the total length of the leg (about 4 cm or 1 2/3 inches in an average adult) may cause noticeable abnormalities when walking. These differences may require the patient to exert more effort to walk. There is controversy about the effect of limb length discrepancy on back pain. Some studies show that people with a limb length discrepancy have a greater incidence of low back pain and an increased susceptibility to injuries. Other studies do not support this finding.
Diagnosis
Infants, children or adolescents suspected of having a limb-length condition should receive an evaluation at the first sign of difficulty in using their arms or legs. In many cases, signs are subtle and only noticeable in certain situations, such as when buying clothing or playing sports. Proper initial assessments by qualified pediatric orthopedic providers can reduce the likelihood of long-term complications and increase the likelihood that less invasive management will be effective. In most cases, very mild limb length discrepancies require no formal treatment at all.
Non Surgical Treatment
A personalized approach to leg length discrepancy treatment works best for each patient. Your child's doctor will consider many factors when deciding on a course of treatment for this condition. Such factors can include your child's age, extent of the leg length discrepancy, medical history, how your child tolerates certain treatments and procedures, your child's health and prognosis, growth rate, and parental preferences. There is no cookie cutter treatment for each child, or even each centimeter of leg difference. Once all of these factors have been carefully considered, your child's physician will come up with an appropriate course of care. In situations of a very small leg length discrepancy, no treatment, only periodic medical evaluation, may be necessary.

how do you grow taller in a week?
Surgical Treatment
Surgical operations to equalize leg lengths include the following. Shortening the longer leg. This is usually done if growth is already complete, and the patient is tall enough that losing an inch is not a problem. Slowing or stopping the growth of the longer leg. Growth of the lower limbs take place mainly in the epiphyseal plates (growth plates) of the lower femur and upper tibia and fibula. Stapling the growth plates in a child for a few years theoretically will stop growth for the period, and when the staples were removed, growth was supposed to resume. This procedure was quite popular till it was found that the amount of growth retarded was not certain, and when the staples where removed, the bone failed to resume its growth. Hence epiphyseal stapling has now been abandoned for the more reliable Epiphyseodesis. By use of modern fluoroscopic equipment, the surgeon can visualize the growth plate, and by making small incisions and using multiple drillings, the growth plate of the lower femur and/or upper tibia and fibula can be ablated. Since growth is stopped permanently by this procedure, the timing of the operation is crucial. This is probably the most commonly done procedure for correcting leg length discrepancy. But there is one limitation. The maximum amount of discrepancy that can be corrected by Epiphyseodesis is 5 cm. Lengthening the short leg. Various procedures have been done over the years to effect this result. External fixation devices are usually needed to hold the bone that is being lengthened. In the past, the bone to be lengthened was cut, and using the external fixation device, the leg was stretched out gradually over weeks. A gap in the bone was thus created, and a second operation was needed to place a bone block in the gap for stability and induce healing as a graft. More recently, a new technique called callotasis is being use. The bone to be lengthened is not cut completely, only partially and called a corticotomy. The bone is then distracted over an external device (usually an Ilizarov or Orthofix apparatus) very slowly so that bone healing is proceeding as the lengthening is being done. This avoids the need for a second procedure to insert bone graft. The procedure involved in leg lengthening is complicated, and fraught with risks. Theoretically, there is no limit to how much lengthening one can obtain, although the more ambitious one is, the higher the complication rate.
Dealing With Mortons Neuroma
 Some sources claim that entrapment of the plantar nerve because of compression between the metatarsal heads, as originally proposed by Morton, is highly unlikely, because the plantar nerve is on the plantar side of the transverse metatarsal ligament and thus does not come in contact with the metatarsal heads. It is more likely that the transverse metatarsal ligament is the cause of the entrapment. Despite the name, the condition was first correctly described by a chiropodist named Durlacher, and although it is labeled a "neuroma", many sources do not consider it a true tumor, but rather a perineural fibroma (fibrous tissue formation around nerve tissue).
Some sources claim that entrapment of the plantar nerve because of compression between the metatarsal heads, as originally proposed by Morton, is highly unlikely, because the plantar nerve is on the plantar side of the transverse metatarsal ligament and thus does not come in contact with the metatarsal heads. It is more likely that the transverse metatarsal ligament is the cause of the entrapment. Despite the name, the condition was first correctly described by a chiropodist named Durlacher, and although it is labeled a "neuroma", many sources do not consider it a true tumor, but rather a perineural fibroma (fibrous tissue formation around nerve tissue).Causes
Some experts believe that other foot conditions may also be associated with Morton's neuroma. This is because other conditions may cause the metatarsal bones to rub against the nerve in your foot. Foot problems that may increase your risk of developing Morton's neuroma include abnormally positioned toes, high arches, where the arch or instep of your foot is raised more than normal, flat feet, low arches or no arches at all, bunions a bony swelling at the base of the toe. Hammer toe, where the toe is bent at the middle joint. Being active and playing sport can make the painful symptoms of Morton's neuroma worse. In particular, running or sports that involve running, such as racquet sports, can place extra pressure on the nerve in your foot, which can aggravate the problem.
Symptoms
Morton?s neuroma is a progressive condition which means the symptoms typically get worse over time. Initially people often complain of a tingling or numbness at the base of their toes, typically in the space between the third and fourth toes, or, less commonly , between the second and third toes, which feels a bit like pins and needles. Over time the pain progresses and can feel like a stabbing or burning sensation in the ball of the foot under the toes. Some describe it as feeling as if they are standing on a stone. Normally the pain will get worse when you wear tight fitting shoes. Doing exercise that impacts on the foot such as jogging can also make the symptoms worse. The extent of the pain varies from person to person but in some cases it can be so intense that every step can feel acutely painful.
Diagnosis
Morton's neuroma is usually diagnosed by your doctor listening to your symptoms and examining your foot. Sometimes your doctor can feel the 'neuroma', or an area of thickening in your foot, which may be tender. Sometimes, your doctor may suggest an ultrasound scan or MRI scan to confirm the diagnosis but this is not always necessary. Some doctors inject a local anaesthetic into the area where you are experiencing pain. If this causes temporary relief of pain, burning and tingling, it can sometimes help to confirm the diagnosis and show the doctor where the problem is.
Non Surgical Treatment
The first step in treating Morton's Neuroma is to select proper footwear. Footwear with a high and wide toe box (toe area) is ideal for treating and relieving the pain. The next step in treatment is to use an orthotic designed with a metatarsal pad. This pad is located behind the ball-of-the-foot to unload pressure, and relieve the pain caused by the neuroma.
If problem persists, consult your foot doctor.

Surgical Treatment
Surgery for mortons neuroma consists of either a decompression, where more space is created for the nerve or a resection, where this part of the nerve is removed completely. This will result in some permanent minor numbness. Success rates for surgical procedures to treat mortons neuroma have a high success rate.
Leg Length Discrepancy And Shoe Lifts

Leg length inequality goes largely undiscovered on a daily basis, yet this problem is easily fixed, and can reduce quite a few instances of back ache.
Treatment for leg length inequality typically consists of Shoe Lifts. Most are affordable, ordinarily being less than twenty dollars, in comparison to a custom orthotic of $200 if not more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Upper back pain is easily the most common ailment affecting people today. Around 80 million men and women have problems with back pain at some point in their life. It's a problem that costs businesses huge amounts of money annually on account of lost time and output. Fresh and superior treatment methods are constantly sought after in the hope of lowering economical influence this condition causes.

Men and women from all corners of the world suffer from foot ache due to leg length discrepancy. In a lot of these cases Shoe Lifts might be of immense help. The lifts are capable of easing any discomfort and pain in the feet. Shoe Lifts are recommended by countless skilled orthopaedic doctors.
So that you can support the body in a well balanced fashion, the feet have a critical role to play. In spite of that, it is often the most neglected zone of the human body. Many people have flat-feet which means there may be unequal force exerted on the feet. This will cause other body parts such as knees, ankles and backs to be affected too. Shoe Lifts guarantee that proper posture and balance are restored.
How To Lessen Hammertoe Pain
 Overview
Overview
A Hammer toes occurs from a muscle and ligament imbalance around the toe joint which causes the middle joint of the toe to bend and become stuck in this position. The most common complaint with hammertoes is rubbing and irritation on the top of the bent toe. Toes that may curl rather than buckle, most commonly the baby toe, are also considered hammertoes. It can happen to any toe. Women are more likely to get pain associated with hammertoes than men because of shoe gear. Hammertoes can be a serious problem in people with diabetes or poor circulation. People with these conditions should see a doctor at the first sign of foot trouble.
Causes
A common cause of hammertoe and mallet toe is wearing improper footwear - shoes that are too tight in the toe box, or high-heel shoes. Wearing shoes of either type can push your toes forward, crowding one or more of them into a space that's not large enough to allow your toes to lie flat. Hammertoe and mallet toe deformities can also be inherited and may occur despite wearing appropriate footwear. The result is a toe that bends upward in the middle and then curls down in a hammer-like or claw-like shape. Your shoes can rub against the raised portion of the toe or toes, causing painful corns or calluses. The bottom of the affected toe can press down, creating the mallet-like appearance of mallet toe. At first, a hammertoe or mallet toe may maintain its flexibility and lie flat when you're not wearing crowded footwear. But eventually, the tendons of the toe may contract and tighten, causing your toe to become permanently stiff.
 Symptoms
Symptoms
Patients with hammer toe(s) may develop pain on the top of the toe(s), tip of the toe, and/or on the ball of the foot. Excessive pressure from shoes may result in the formation of a hardened Hammer toe portion of skin (corn or callus) on the knuckle and/or ball of the foot. Some people may not recognize that they have a hammer toe, rather they identity the excess skin build-up of a corn.The toe(s) may become irritated, red, warm, and/or swollen. The pain may be dull and mild or severe and sharp. Pain is often made worse by shoes, especially shoes that crowd the toes. While some hammer toes may result in significant pain, others may not be painful at all. Painful toes can prevent you from wearing stylish shoes.
Diagnosis
A hammertoe is usually diagnosed with a physical inspection of your toe. Imaging tests, such as X-rays, may be ordered if you have had a bone, muscle, or ligament injury in your toe.
Non Surgical Treatment
Conservative treatment starts with new shoes that have soft, roomy toe boxes. Shoes should be one-half inch longer than your longest toe. (Note: For many people, the second toe is longer than the big toe.) Avoid wearing tight, narrow, high-heeled shoes. You may also be able to find a shoe with a deep toe box that accommodates the hammer toe. Or, a shoe specialist (Pedorthist) may be able to stretch the toe box so that it bulges out around the toe. Sandals may help, as long as they do not pinch or rub other areas of the foot.
Surgical Treatment
In more advanced cases of hammer toe, or when the accompanying pain cannot be relieved by conservative treatment, surgery may be required. Different types of surgical procedures are performed to correct hammer toe, depending on the location and extent of the problem. Surgical treatment is generally effective for both flexible and fixed (rigid) forms of hammer toe. Recurrence following surgery may develop in persons with flexible hammer toe, particularly if they resume wearing poorly-fitted shoes after the deformity is corrected.
Could Hammertoes Induce Leg Soreness
 Overview
Overview
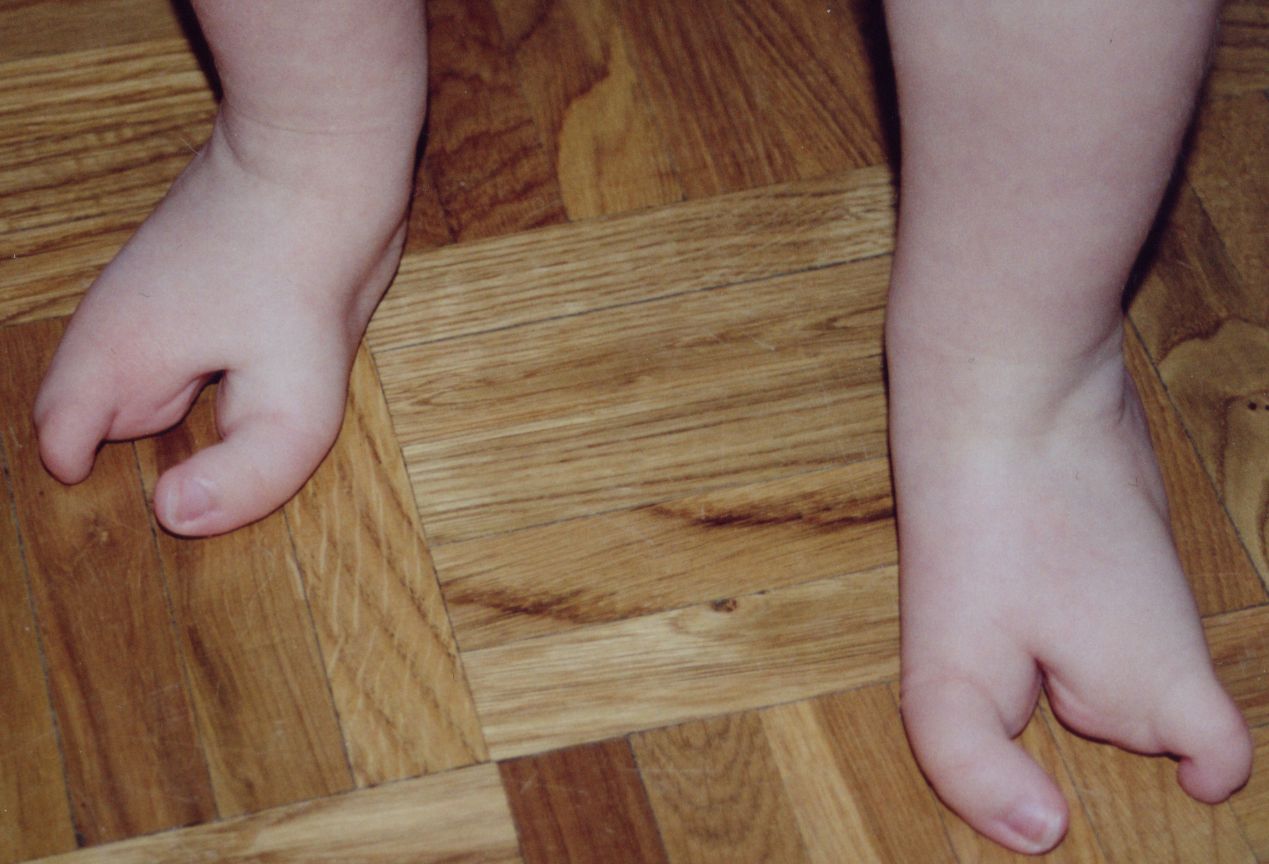
Hammertoe is a secondary problem originating from fallen cross arches. The toes start to curl and get pulled backwards, as the collapsed or pushed out metatarsal bones pull the tendons and ligaments, and causes them to get shorter and tighter. This condition causes the toes have higher pressure and they have limited movement and cannot be straightened fully. This can lead to numbness and pain in the toes as muscles, nerves, joints and little ligaments are involved with this condition. As the top part of the toe can rub against the shoe, it can cause corns and calluses.
Causes
Essentially, hammertoes are caused by an abnormal interworking of the bones, muscles, ligaments and tendons that comprise your feet. When muscles fail to work in a balanced manner, the toe joints can bend to form the hammertoe shape. If they remain in this position for an extended period, the muscles and tendons supporting them tighten and remain in that position. A common factor in development of hammertoe is wearing shoes that squeeze the toes or high heels that jam the toes into the front of the shoe. Most likely due to these factors, hammertoe occurs much more frequently in women than in men. 
Symptoms
Hammer, claw, and mallet toes can cause discomfort and pain and may make it hard to walk. Shoes may rub on your toes, causing pain, blisters, calluses or corns, or sores. Sores can become infected and lead to cellulitis or osteomyelitis, especially if you have diabetes or peripheral arterial disease. If you have one of these health problems and sores develop, contact your doctor.
Diagnosis
Your doctor is very likely to be able to diagnose your hammertoe simply by examining your foot. Even before that, he or she will probably ask about your family and personal medical history and evaluate your gait as you walk and the types of shoes you wear. You'll be asked about your symptoms, when they started and when they occur. You may also be asked to flex your toe so that your doctor can get an idea of your range of motion. He or she may order x-rays in order to better define your deformity.
Non Surgical Treatment
Wear wide shoes with plenty of room in the toes and resilient soles. Avoid wearing shoes with pointed toes. Commercially available felt pads or cushions may ease pressure from the shoe on the toe. Toe caps (small, padded sleeves that fit around the tip of the toe) may relieve the pain of hammer toe. Do toe exercises, to help toe muscles become stronger and more flexible. Arch supports or an orthotic shoe insert prescribed by your doctor or podiatrist may help to redistribute weight on the foot. These devices do not cure the problem but may ease the symptoms of either hammer toe or mallet toe.
Surgical Treatment
Sometimes when the joints are removed the two bones become one as they are fused in a straightened position. Many times one toe will be longer than another and a piece of bone is removed to bring the toes in a more normal length in relation to each other. Sometimes tendons will be lengthened, or soft tissue around the joints will be cut or rebalanced to fix the deformity. Angular corrections may also be needed. The surgeon may place fixation in your foot as it heals which may include a pin, or wires. 
Prevention
Good circulation is essential. When you're sitting down, put your feet up. If you've been sitting for a while, stretch your legs and feet. Give yourself a foot massage or trade foot massages with someone you love. A warm foot bath is also a good idea. Most people have one foot that's bigger than the other. Fit your shoes to the bigger foot. Buy shoes at the end of the day, as feet tend to swell a bit and you will get a better sense of fit. When buying shoes, wear the socks that you will be using when wearing that shoe. For example, wear an athletic sock when buying athletic shoes and a dress sock when purchasing dress shoes. If the shoe does not feel good at the time of purchase, then it will never feel good.